Case Report | DOI: https://doi.org/10.31579/2692-9392/065
Pesky Hiccups; May be Risky!
- Abeer M Shawky 1*
*Corresponding Author: Abeer M Shawky, Consultant Non-invasive Cardiology Faculty of Medicine, Al-Azhar University, Cairo, Egypt
Citation: Abeer M Shawky (2021) Pesky Hiccups; May be Risky!. J. Archives of Medical Case Reports and Case Study. 4(3); DOI:10.31579/2692-9392/065
Copyright: © 2021 Abeer M Shawky, This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 18 June 2021 | Accepted: 16 July 2021 | Published: 21 July 2021
Keywords: coronary heart disease; hiccups; myocardial infarction
Abstract
Background: Hiccups are benign and self-limited condition, but attention should be paid to the underlying conditions when persist. There are various causes of persistent hiccups, including metabolic abnormalities, psychogenic disorders, malignancy, nervous system pathology, medications, pulmonary disorders, or gastrointestinal etiologies. It is rarely attributed to cardiac disease.
Case Summary: We report a case of intractable hiccups in a 67 y/o male as the initial symptom of coronary heart disease. He presented with a few-week history of hiccups and no other complaints. Echocardiography demonstrated wall motion abnormalities in the left ventricle with severe impairment of systolic function. He was He was admnistered chlorpromazine and anti-ischemic treatment, and a thallium viability study was advised before cardiac catheterization to confirm viable or nonviable myocardium. He refused further evaluation and was discharged with appropriate care. The gentleman was readmitted for heart failure two weeks after discharge due to poor medication adherence. The delay in treatment had affected his chances of survival, and his hiccuping symptoms had recurred and persisted. Finally, he died after two months from the time of diagnosis.
Discussion: This case makes highlights the importance of having a high index of suspicion, especially in elderly diabetic patients where benign self-limiting conditions like hiccups can only present symptoms of severe cardiac disease. Cardiac disease should be considered even when the symptoms are only gastrointestinal; simple investigations in the form of changes in electrocardiogram with cardiac enzyme elevation may disclose the cardiac findings, as they did in our case!
Learning Points
- Pesky hiccups may be risky.
- Myocardial infarction/ischemia-induced hiccups are very rare and cause delayed diagnosis.
- Physicians should be alert to the possibility of an atypical presentation and unusual symptomatology for coronary artery disease in patients who present with persistent hiccups.
Background
Hiccups are involuntary, paroxysmal inspiratory movements of the chest wall associated with diaphragm and accessory respiratory muscle contractions, with sudden inhalation and subsequent spasmodic closure of the glottis with abrupt air rush into lungs causing a little “hic” sound [1]. We think of hiccups as annoying but not serious; that might not always be the case; pesky hiccups may be risky. Hiccups can be associated with underlying medical conditions if they continue for more than a day [2]. We herein report a case of persistent hiccups as the initial symptom of coronary heart disease.
Case Summary
The current patient was a 67-year-old man who presented to the emergency department with a 6-week history of hiccups and a poor appetite. According to the patient description, these pesky hiccups increased in intensity, aggravated by lying supine and preventing sleep at night. The patient could barely eat anything and felt weak as he noted that; eating would worsen the hiccups, and epigastric pain later developed. The patient denied typical chest pain or other angina equivalents at any time. The patient on admission was hemodynamically stable but a little bit asleep. His blood pressure was 110/65 mmHg, heart rate was 100 beats per minute and regular, body temperature was 37.1°C, respiratory rate was 12 breaths per minute, and oxygen saturation was 98% while breathing room air. Cardiac auscultation revealed heart sounds without murmurs. The abdomen was non-tender with no guarding or rigidity. He had a medical history of diabetes, hyperlipidemia, gastritis and chronic obstructive pulmonary disease due to chronic tobacco use.
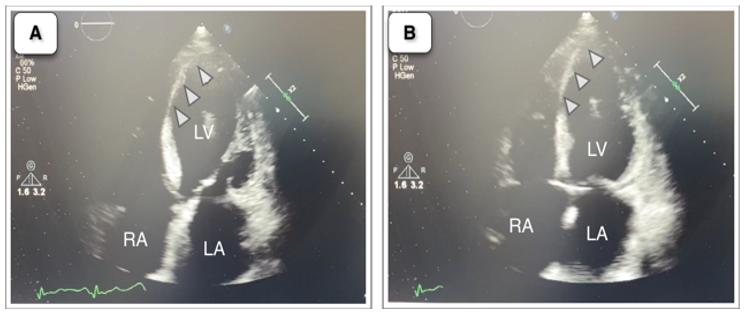
Laboratory tests were significant for a white cell count of 10.7 per cubic millimetre with 85.9% neutrophils. C-reactive protein level was 6.78 mg/dL. Thyroid-stimulating hormone was 10.8 IU/mL. Creatinine level was 2.4 mg/dL. Upper abdominal ultrasonography revealed grade I nephropathy, mildly enlarged liver with a typical homogenous echo pattern. Chest radiography demonstrated an increase in cardiothoracic ratio with evidence of mild pulmonary congestion (Figure 1). A 12-lead electrocardiogram (ECG) displayed sinus tachycardia, low voltage in limb leads with pathological Q waves in inferior leads without ST-segment elevation. Left atrial enlargement with left axis deviation was also present. The cardiac troponin-I peaked at 533.1 pg/mL (reference value < 26>(Figure 2). With follow up of his laboratory results, he was found to have more renal impairment.
Our patient started chlorpromazine, aspirin, clopidogrel, low molecular weight heparin, nitroglycerin, atorvastatin, furosemide and bisoprolol. Troponin started to trend down with complete resolution of hiccups. After the resolution of acute kidney injury, the patient was advised to do a thallium viability study before diagnostic coronary angiography to confirm viable or nonviable myocardium. He refused any further evaluation; hence, he was discharged with appropriate care. Unfortunately, his hiccups had recurred and persisted, and the patient died after two months from the time of diagnosis.
Discussion
Hiccups are transient and self-limiting and do not present a clinical issue. Pesky hiccups are classified according to the duration of acute attack for less than two days, persistent hiccups for more than two days and intractable hiccups for more than a month. Persistent and intractable hiccups are generally associated with underlying medical conditions [3]. We discussed a case of a 67-year-old gentleman with intractable hiccups as a secondary symptom of myocardial ischemia.
Patients with myocardial infarctions usually present with chest pain and shortness of breath. The case described here included no one of classic descriptions and instead presented with a seemingly benign condition. The persistence of symptoms in our patient eventually warranted a more thorough investigation that resulted in an unexpected diagnosis—a myocardial infarction presenting with hiccups. None of the guidelines mentioned persistent hiccups as a symptom of an acute coronary syndrome (ACS), and myocardial ischemia had been reported in very few cases in the literature to cause hiccups [4]. Shi-Min Yuan, in 2019 stated that hiccups as an only presentation of acute myocardial infarction might be misdiagnosed as gastrointestinal disorders on many occasions [5]. Davenport et al., in 2012, reported a case presented with persistent hiccups without any other cardiac complaints and found to have inferior wall myocardial infarction and diagnostic coronary angiography revealed significant stenosis of the left circumflex and first obtuse marginal coronary arteries [6].
This unusual presentation appears to be important in the diabetic and elderly as those individuals prone to an atypical presentation of ACS [7]. Although our patient did not have any cardiac symptoms to suggest ACS, he had multiple risk factors for coronary artery disease. By revising the limited number of patients in the literature, Shaikh and others in 2018 stated that; most cases of myocardial ischemia presenting with hiccups as the sole symptom have occurred in males with risk factors such as hypertension and diabetes [8]. Our patient was an elderly male with type 2 diabetes, hypertension, hyperlipidemia, and chronic smoking.
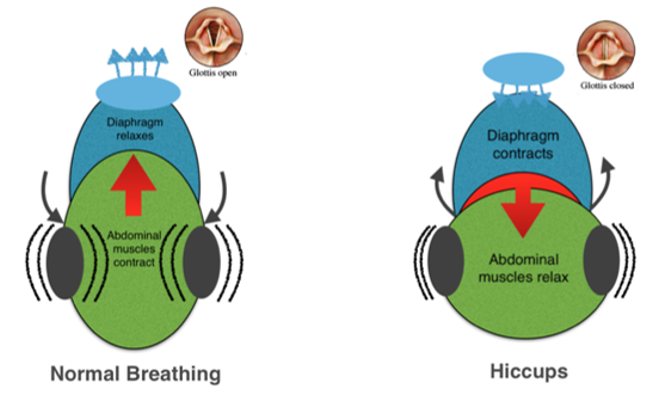
When Hiccups happen, vocal cords quickly close, causing inhalation to be cut short with abrupt inspiration leading to a sharp rush of air into the lungs (Figure 3).
This mechanism plays a vital role in protecting airways against oesophageal aspiration. Hiccups occur during eating too quickly (or too much), drinking alcohol or carbonated beverages, eating something hot or spicy, abdominal surgery, certain medications, or even feeling nervous [3].
Hiccups occur as an involuntary reaction likely related to stimulation of a
reflex arc (Hiccups reflex arc) (Figure 4) that has three components: the afferent limb (vagus and phrenic nerve and thoracic segments of the sympathetic chain; sympathetic fibres from T6-10); followed by a centre in the mid-brain; and finishes with the efferent limb (phrenic nerves supplying the diaphragm and intercostal nerves supplying the intercostal muscle fibres) [9].
Stimulation of any part of the hiccups reflex pathway can lead to hiccups. Stimulants of intractable hiccups are various, including the central nervous system, gastrointestinal tract, abnormal masses, infections, and metabolic aberrations. Heart diseases as myocardial infarction and pacemaker lead injury may cause vagus nerve irritation with subsequent hiccups [10]. Rueckert and Willersinn in 2020 stated that the inflammatory markers released by the acutely ischemic myocardium might trigger the pathway and produce hiccups. The proximity of the heart to the phrenic nerve may lead to either the irritation of the vagus nerve supplying the pericardium or the phrenic nerves, which innervates the diaphragm [11].
In our patient, there were pathological Q waves in inferior leads in his presenting ECG with significant elevated cardiac troponin-I level indicating recent inferior myocardial infarction (MI). In 2008 Krysiak and others presented a case of inferior wall MI with hiccups. In their case, both the right coronary artery (RCA) and left anterior descending artery (LAD) had been significantly obstructed, but the symptom of hiccups was observed to dissipate after the opening of RCA even though LAD remained obstructed [5]. All the published literature about intractable hiccups and myocardial ischemia has shown that hiccups occurred more frequently in patients with inferior and right ventricular infarction than infarctions of other territories [12]. This finding may be because the anatomical distribution of vagal fibres of the cardiac plexus is within the inferoposterior myocardium and phrenic nerve, which provide motor fibres to the diaphragm. The irritation from the infarct or ischemic area may result in stimulation of these fires and cause hiccups. Also, irritation of phrenic nerves, which innervates the diaphragm, can cause persistent hiccups in those patients [13]. Therefore, physicians shall consider the extension of infarction to the inferior wall if a patient with an otherwise stable myocardial infarction develops hiccups [14]. We can state that intractable hiccups in the current patient were likely due to myocardial ischemia that irritated the vagal nerve, which provided parasympathetic innervation to the heart and carried afferent nerve fibres (phrenic) of the hiccup reflex, innervating the diaphragm and causing hiccups.
Effective treatment of persistent hiccup may be established upon the correct diagnosis of causes responsible for this serious event and treatment of this cause. Our patient hiccuped continuously for more than one month despite chlorpromazine and optimal anti-ischemic medications till he died without controlling this pesky hiccup. We tried all pharmacological approaches that failed to control his hiccups may have needed complete revascularization because of ongoing myocardial ischemia. Unfortunately, our patient's refusal to proceed with further diagnostics and treatment leaves this case insufficient in important diagnostics data, which could provide evidence-based connection of hiccups with underlying conditions.
Conclusion
Our case is one of few cases in the literature in which myocardial infarction presented with intractable hiccups as the sole presenting complaint. Therefore, physicians should be attentive to the possibility of an atypical presentation in patients with precipitating factors for coronary artery disease, and elderly patients who present with persistent hiccups should be investigated for an underlying cardiac aetiology.
Acknowledgements
The author would like to thank all medical staffs who shared in treating the patient and providing supports.
Funding:
None.
Disclosures
None.
Consent
Written informed consent was obtained from the patient’s relative to publishing this case report and accompanying images.
References
- Steger M, Schneemann M, Fox M. Systemic review: the pathogenesis and pharmacological treatment of hiccups. Aliment Pharmacol Ther. 2015; 42: 1037-1050.
View at Publisher | View at Google Scholar - Kohse EK, Hollmann MW, Bardenheuer HJ, Kessler J. Chronic Hiccups: An Underestimated Problem. Anesth Analg. 2017; 125: 1169-1183.
View at Publisher | View at Google Scholar - Chang FY and Lu CL. “Hiccup: mystery, nature and treatment” Journal of Neurogastroenterology and Motility. 2012; 18 (2):123–130.
View at Publisher | View at Google Scholar - Krysiak W, Szabowski S, Stepień M, et al: Hiccups as a myocardial ischemia symptom. Pol Arch Med Wewn. 2008; 118(3): 148–151
View at Publisher | View at Google Scholar - Shi-Min Yuan. Myocardial Ischemia Presenting with Hiccups. Journal of the College of Physicians and Surgeons Pakistan. 2019; 29 (5): 469-473
View at Publisher | View at Google Scholar - Davenport J, Duong M, and Lanoix R. “Hiccups as the only symptom of non-ST-segment elevation myocardial infarction.” American Journal of Emergency Medicine, vol. 30, no. 1, pp. 266.e1–266.e2, 2012.
View at Publisher | View at Google Scholar - Kumar A and Cannon CP. “Acute coronary syndromes: diagnosis and management, part II” Mayo Clinic Proceedings. 2009, 84 (11): 1021–1036.
View at Publisher | View at Google Scholar - Shaikh N, Raj R, Movva S, et al. Persistent hiccups as the only presenting symptom of ST-elevation myocardial infarction. Case Rep Cardiol. 2018; 7237454.
View at Publisher | View at Google Scholar - Becker DE. “Nausea, vomiting, and hiccups: a review of mechanisms and treatment” Anesthesia Progress. 2010; 57 (4): 150–157.
View at Publisher | View at Google Scholar - Zhang F, Tongo ND, Hastings V, et al. “ST-segment elevation myocardial infarction with acute stent thrombosis presenting as intractable hiccups: an unusual case” American Journal of Case Reports. 2017; 18,: 467–471.
View at Publisher | View at Google Scholar - Rueckert KK and Willersinn A. Case Report: From Irregular Hiccups to Acute Myocardial Infarction. Perm J. 2020; 25: 20.180
View at Publisher | View at Google Scholar - Culic V, Miric D, Eterovic D. Correlation between symptomatology and site of acute myocardial infarction. Int J Cardiol. 2001; 77:163-168.
View at Publisher | View at Google Scholar - Howes D. Hiccups: A new explanation for the mysterious reflex. Bioessays. 2012; 34 (6): 451-453
View at Publisher | View at Google Scholar - Senthilkumaran S, Meenakshisundaram R, Suresh P, Thirumalaikolundusubramanian P. A hitch in hiccups. Am J Emerg Med. 2012; 30:820-821.
View at Publisher | View at Google Scholar
Dear Grace Pierce, Editorial Coordinator of Journal of Clinical Research and Reports, Thank you for the speedy and efficient peer review process. I appreciate the fact that your peer reviewers do not take months to respond like with some other journals. I would also like to thank the editorial office for responding quickly to my questions. It is an excellent journal. I plan to submit more manuscripts in the future. Best wishes from, Robert W. McGee

Robert W McGee
Dear Grace Pierce, Editorial Coordinator of Journal of Clinical Research and Reports, Working with you and your team on our recent publication in JCRR has been a truly wonderful and enjoyable experience. The responses were prompt, and the reviewers were patient, constructive, and highly professional. One reviewer in particular gave me the feeling that a professor was carefully reading and commenting on my coursework, which was deeply touching. The entire process was straightforward and hassle‑free, with no tedious online forms to complete. I highly recommend this journal. Best wishes from, DR Aibing Rao, Head of R&D

Aibing Rao
I Appreciate the Opportunity to Share my Experience with the Journal of Clinical Research and Reports. The peer review process was timely and constructive, and the feedback provided helped improve the quality of our manuscript. The editorial office was professional, responsive, and supportive throughout the process, ensuring smooth communication and efficient handling of the submission. Overall, it was a positive experience collaborating with your team.

Kashani Mehdi
Dear Mercy Grace, Editorial Coordinator of Obstetrics Gynecology and Reproductive Sciences, We would like to express our gratitude for your help at all stages of publishing and editing the article. The editors of the magazine answer all the necessary questions and help at every stage. We will definitely continue to cooperate and publish other works in the Obstetrics Gynecology and Reproductive Sciences! Best wishes from, Alla Konstantinovna Politova,

Alla Konstantinovna Politova
Dear Maria Emerson, Editorial Coordinator of International Journal of Clinical Case Reports and Reviews, What distinguishes International Journal of Clinical Case Report and Review is not only the scientific rigor of its publications, but the intellectual climate in which research is evaluated. The submission process is refreshingly free of unnecessary formal barriers and bureaucratic rituals that often complicate academic publishing without adding real value. The peer-review system is demanding yet constructive, guided by genuine scientific dialogue rather than hierarchical or authoritarian attitudes. Reviewers act as collaborators in improving the manuscript, not as gatekeepers imposing arbitrary standards. This journal offers a rare balance: high methodological standards combined with a respectful, transparent, and supportive editorial approach. In an era where publishing can feel more burdensome than research itself, this platform restores the original purpose of peer review — to refine ideas, not to obstruct them Prof. Perlat Kapisyzi, FCCP PULMONOLOGIST AND THORACIC IMAGING.
Perlat Kapisyzi
Dear Reader: We have published several articles in the Auctores Publishing, LLC, journal, Clinical Medical Reviews and Reports in recent years (CMRR). This is an ‘open access’ journal and the following are our observations. From the initial invitation to submit an article, to the final edits of galley proofs, we have found CMRR personnel to be professional, responsive, rapid and thorough. This entire process begins with Catherine Mitchell, Editorial Coordinator. She is simply outstanding, and, I believe, unparalleled in her capacity. I cannot imagine a more responsive and dedicated Editorial Coordinator. As I read the dates and timing of her correspondence with us, it seems that she never sleeps. I hope Auctores Publishing, LLC, appreciates her efforts as much as these authors do. Thank you to Auctores Publishing, LLC, to the Editorial Staff/Board, and to Catherine Mitchell from a grateful author(s).