Case Report | DOI: https://doi.org/10.31579/2693-2156/027
Arrhythmogenic anterior myocardial infarction with QRS-complex fragmentations and Passing phenomenon or Yasser’s phenomenon; the risk and serious implications
- Yasser Mohammed Hassanain Elsayed *
* Critical Care Unit, Al-Rodah Central Hospital, Damietta Health Affairs, Egyptian Ministry of Health (MOH), Damietta, Egypt.
*Corresponding Author: Yasser Mohammed Hassanain Elsayed, Critical Care Unit, Al-Rodah Central Hospital, Damietta Health Affairs, Egyptian Ministry of Health (MOH), Damietta, Egypt.
Citation: Elsayed Y M H, (2021). Arrhythmogenic anterior myocardial infarction with QRS-complex fragmentations and Passing phenomenon or Yasser’s phenomenon; the risk and serious implications. J Thoracic Disease and Cardiothoracic Surgery, 2(3); DOI:10.31579/2693-2156/027
Copyright: © 2021, Elsayed Y M H. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 04 September 2021 | Accepted: 17 September 2021 | Published: 28 September 2021
Keywords: arrhythmia; anterior myocardial infarction; QRS-complex fragmentations; passing phenomenon or yasser’s phenomenon; PVCS; AF
Abstract
Rationale: The arrhythmias associated with myocardial infarction may be serious. Increasing morbidity and mortality in myocardial infarction-induced arrhythmias will be expected. The term “fragmentation of the QRS complex” denotes the existence of high-frequency potentials (spikes) in the QRS-complex. It is either a marker for cardiac structural diseases inducing biventricular hypertrophy or any condition interfering with the normally homogeneous depolarization status inside the myocardium. An associated Passing phenomenon or “Yasser’s phenomenon” may have an apparent hemodynamic impact. Patient concerns: A 68-year-old married, housewife, Egyptian female patient presented to the physician outpatient clinic with acute chest pain and anterior myocardial infarction with QRS-complex fragmentations and Passing phenomenon or “Yasser’s phenomenon”. Diagnosis: Arrhythmogenic acute extensive anterior infarction with QRS-complex fragmentations and Passing phenomenon or Yasser’s phenomenon. Interventions: Electrocardiography, oxygenation, streptokinase intravenous infusion, echocardiography, and percutaneous transluminal coronary angioplasty. Outcomes: Dramatic response of acute arrhythmogenic anterior ST-segment elevation myocardial infarction with QRS-complex fragmentations to streptokinase and percutaneous transluminal coronary angioplasty. Lessons: The presence of runs of ventricular tachycardia, multiform frequent premature ventricular contractions, and QRS-complex fragmentations, elderly, female sex are prognostic factors for the severity of the disease. Dramatic clinical and electrocardiographic response signifying the role of streptokinase, fibrinolytic, and percutaneous transluminal coronary angioplasty. The presence of fragmentation of the QRS-complex may have a bidirectional impact from seriousness to complications. Passing phenomenon or “Yasser’s phenomenon” should be directed at the disease progression.
Introduction
The common arrhythmias associated with anterior myocardial infarction are supraventricular (SVT) and ventricular tachycardia (VT) [1]. Sudden cardiac death (SCD) due to arrhythmia after myocardial infarction (MI) may be predicted and avoided in certain situations [1]. The risk of SCD due to malignant arrhythmia such as VT must be considered in patients with structural heart disease (SHD) who have frequent premature ventricular contractions (PVCs) [2]. High-frequency PVCs have an adversely poor prognosis [3]. Multifocal PVCs are red flags and risk markers for SCD [4]. Myocardial infarction (MI) remains the leading cause of death throughout the world. Ischemic heart disease (IHD) has been a significant cause of morbidity throughout the world for decades [5]. Anterior myocardial infarction (AMI) is a common cardiac disease accompanied by remarkable mortality and morbidity. Development in diagnosis and management options have a role in favorable outcome [6]. Classification of AMI is based on ECG findings as follows [7]:
1. Anteroseptal; ST-segment elevation in leads V1- V4
2. Anteroapical (or mid-anterior); ST-segment elevation in leads V3-V4
3. Anterolateral; ST-segment elevation in leads V3- V6
4. Extensive anterior; ST-segment elevation in leads V1- V6.
Optimal treatment approaches are based on the pathophysiology of the infarct and the presence of precipitating factors (eg, chronic heart failure, metabolic diseases) [1]. The term ‘fragmentation of the QRS-complex” or “fragmented QRS” (fQRS) point to the existence of high-frequency potentials (spikes) in the QRS-complex [8]. The expression was first described in 1973 in reporting of an experimental study on canine hearts where coronary artery obstruction motivated the occurrence of fragmented electrograms as a source of reentrant activity [9]. Formerly, fQRS had already been considered a marker for SHD triggering biventricular hypertrophy [10]. The presence of fQRS can be induced by any condition interrupting with the normally homogeneous depolarisation status in the myocardium and yielding regional conduction decelerating such as ischemia, scar, fibrosis, myofiber disarray, inflammation, and microvascular abnormality [8]. Das et al. revealed that there was a good correlation between fQRS and the presence of myocardial scar in patients with ischemic heart disease (IHD) that appeared by single-photon emission tomography (SPET) [11]. The new “Passing phenomenon” is a transient electrocardiographic change that spontaneously reversed within a few seconds to a few minutes without any medical interventions and apparent hemodynamic impact. Reassurance is immediate therapy. The electrophysiological study is the future advised investigation [12].
Case Presentation
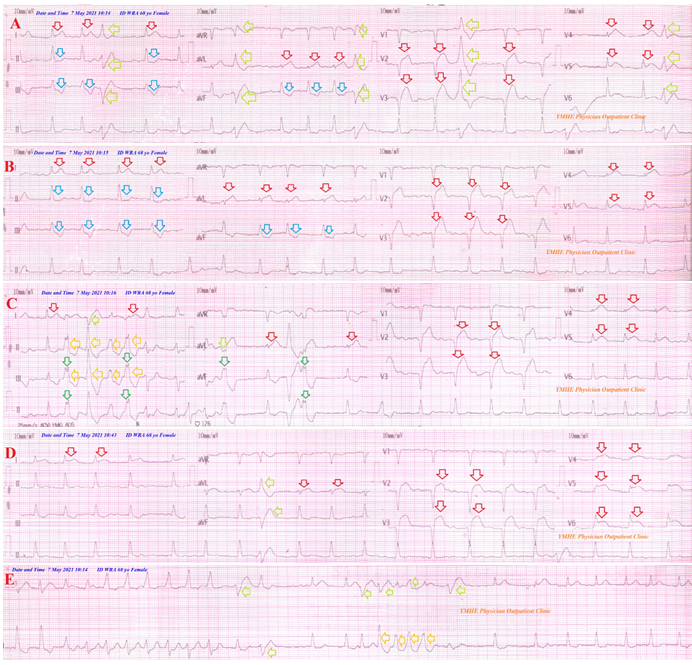
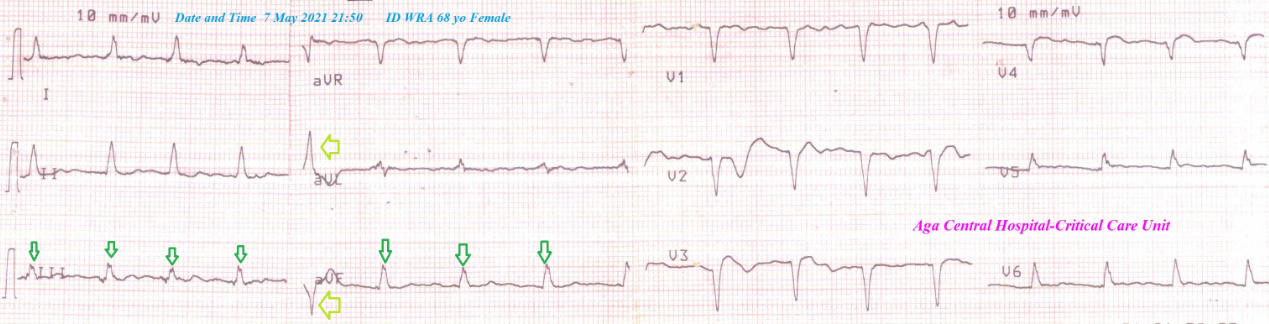
A 68-year-old married, housewife, Egyptian female patient presented to physician outpatient clinic (POC) with acute severe chest pain and palpitations. Profuse sweating and dyspnea were the only accompanied symptoms. She denied a history of cardiovascular diseases, the same attack, drugs, or any other special habits. Chest pain was anginal, compressible, intolerable, and progressive. Informed consent was taken. Upon general physical examination; generally, the patient was anxious, severe sweaty, had cold extremities, with an irregular heart rate of 120 bpm, blood pressure of 130/70 mmHg, respiratory rate of 20 bpm, the temperature of 36.8 °C, and pulse oximeter of O2 saturation of 94%. No more relevant clinical data were noted during the clinical examination. Urgent and serial ECG tracings were done in the POC. The initial ECG tracing showing an acute extensive anterior (I, aVL, and V2-V5) ST-segment elevation myocardial infarction and reciprocal ST-depression changes in leads (II, III, and aVF). There are multiple multi-formed PVCs and atrial fibrillations (AF). (Figure 1A). The second ECG tracing was done within 1 minute of the initial above tracing showing the same of the above tracing but there was no PVCS (Passing phenomenon or Yasser’s phenomenon) (Figure 1B). The third ECG tracing was done within 2 minutes of the initial above tracing showing like the initial tracing but there are QRS fragmentations in (III and aVF) leads. There are also runs of VT. (Figure 1C). Aspirin 4 chewable oral tablet (75 mg), clopidogrel 4 oral tablet (75 mg), O2 inhalation was given (100%, by nasal cannula, 5L/min) were the emergency given medications in the POC before hospital referral. The third ECG tracing was done within 30 minutes of the above emergency given medications showing normalization of most of the above PVCs and QRS fragmentations. (Figure 1D). The patient was referred by ambulance to the nearest central hospital. She was admitted to the ICU for anginal chest pain. Arrhythmogenic acute extensive anterior infarction with QRS-complex fragmentations and Passing phenomenon or Yasser’s phenomenon was the most probable diagnosis. Pethidine HCL 100 mg given on intermittent IV doses, streptokinase IVI (1.5 million units over 60 minutes) bisoprolol oral tablet (5mg) were given in the ICU. The chest pain is still present. The patient was referred from ICU to catheterization lab center for emergency PCI. Clinical improvement and gradual electrocardiographic ST-segment (whether elevations or reciprocal ST-depressions) resolution had happened. ECG tracing was done within 10 hours of ICU admission and after giving streptokinase showing resolution of ST-segment elevation, AF of VR; 100 bpm, PVCs, and are QRS fragmentations in (III and aVF) leads (Figure 2). The measured random blood sugar was 145 mg/dl. The troponin test was positive (2.26 ng/L). The patient had undergone to cardiac catheter within 12 hours of presentations which showed normal left main artery, atherosclerotic totally obstructed LAD, atherosclerotic LCX with no significant lesion, and atherosclerotic dominant RCA with no significant lesion. Two DES were applied. No more workup was done. The patient was continued: aspirin tablet (75 mg, once daily), clopidogrel tablet (75 mg, once daily), bisoprolol oral tablet (5mg, once daily), warfarin tablet (3 mg, once daily; with INR adjustment), and atorvastatin (40 mg once daily). Future cardiovascular follow-up was advised.
Discussion
• Overview:
• A 68-year-old married, housewife, Egyptian female patient presented to the physician outpatient clinic with acute severe chest pain and anterior ST-segment elevation myocardial infarction (STEMI) with QRS-complex fragmentations, and Passing phenomenon or “Yasser’s phenomenon”.
• The primary objective for my case study was the presence of a patient who presented with acute anterior STEMI with QRS-complex fragmentations, and a Passing phenomenon or “Yasser’s phenomenon” in the POC.
• The secondary objective for my case study was the question of; How did you manage the case at home?
• There is an existence of lonely extensive acute anterior ST-segment elevation myocardial infarction.
• The presence of runs of ventricular tachycardia and multiform frequent premature ventricular contractions (PVCs) were associated with acute STEMI.
• There is the presence of fragmentation of the QRS-complex in the is considered another risk.
• Dramatic clinical ECG reversal of ST-segment deviations after streptokinase and initial emergency medications is a good prognostic sign.
• The improvement in clinical and electrocardiographic findings after PTCA and medical treatment strengthen their role in the management of the current case.
• The dramatic disappearance of the QRS-complex fragmentations and Passing phenomenon or “Yasser’s phenomenon” after giving oral aspocid, oral clopidogrel, and nasal 100 % O2 set was the signifying their effects in the current case study.
• Massive acute pulmonary embolism (APE) is the most possible differential diagnosis for the current case study.
• I can’t compare the current case with similar conditions. There are no similar or known cases with the same management for near comparison.
• There are no known limitations of the current study.
Conclusion
• The presence of runs of ventricular tachycardia, multiform frequent premature ventricular contractions, and QRS-complex fragmentations, elderly, female sex are prognostic factors for the severity of the disease.
• Dramatic clinical and electrocardiographic response signifying the role of streptokinase, fibrinolytic, and percutaneous transluminal coronary angioplasty.
• The presence of fragmentation of the QRS-complex may have a bidirectional impact from seriousness to complications.
• Passing phenomenon or “Yasser’s phenomenon” should be directed at the disease progression.
Acknowledgement
• The author wishes to thank my wife to save time and improving the conditions for supporting me.
Conflicts of Interest
• There are no conflicts of interest.
Abbreviations
AMI: Anterior myocardial infarction
ECG: Electrocardiogram
fQRS: Fragmented QRS
ICU: Intensive care unit
LAD: Left anterior descending
PTCI: Percutaneous transluminal coronary angioplasty
PVCs: Premature ventricular contractions
RCA: Right coronary artery
SCD: Sudden cardiac death
SHD: Structural heart diseases
STEMI: ST-segment elevation myocardial infarction
VT: Ventricular tachycardia
References
- Granrud GA, Vatterott PJ. Arrhythmias and acute myocardial infarction. Postgrad Med. 1991 Nov 1;90(6):85-8, 93-96.
View at Publisher | View at Google Scholar - Silva AP, Merino JL. (2011). Frequent ventricular extrasystoles: significance, prognosis and treatment. E-Journal of the ESC Council for Cardiology Practice. 2011 Jan 28;9(17).
View at Publisher | View at Google Scholar - Latchamsetty R, Bogun F. (2016). Premature Ventricular Complex-induced Cardiomyopathy. Rev Esp Cardiol. 2016 April;69(4):365-369.
View at Publisher | View at Google Scholar - Elsayed YMH. (2019). Premature Ventricular Contractions from Benign to Seriousness-A Narrative Updating Review. Archives of Emergency Medicine and Intensive Care. 2019;2(12):1-21.
View at Publisher | View at Google Scholar - Bozbeyoğlu E, Aslanger E, Yıldırımtürk Ö, Şimşek B, Hünük B, Karabay CY, Kozan Ö, Değertekin M. (2019). The established electrocardiographic classification of anterior wall myocardial infarction misguides clinicians in terms of infarct location, extent and prognosis. Ann Noninvasive Electrocardiol. 2019 May; 24(3):e12628.
View at Publisher | View at Google Scholar - Bansal K, Gore M, Nalabothu P. (2021). Anterior Myocardial Infarction. [Updated 2021 Jul 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan.
View at Publisher | View at Google Scholar - Thygesen K, Alpert JS, Jaffe AS, Chaitman BR, Bax JJ, Morrow DA, White HD. (2018). Executive Group on behalf of the Joint European Society of Cardiology (ESC)/American College of Cardiology (ACC)/American Heart Association (AHA)/World Heart Federation (WHF) Task Force for the Universal Definition of Myocardial Infarction. (2018). Fourth Universal Definition of Myocardial Infarction (2018). Circulation. 2018 Nov 13;138(20):e618-e651. Erratum in: Circulation. 2018 Nov 13;138(20):e652.
View at Publisher | View at Google Scholar - Brohet C. (2019). Fragmentation of the QRS complex: the latest electrocardiographic craze? Editorial, Acta Cardiologica. 2019;74(3):185-187.
View at Publisher | View at Google Scholar - Boineau JP, Cox JL. (1973). Slow ventricular activation in acute myocardial infarction. A source of re-entrant premature ventricular contractions. Circulation. 1973;48:702–713.
View at Publisher | View at Google Scholar - Flowers NC, Horan LG, Thomas JR, et al. (1969). The anatomic basis for high-frequency components in the electrocardiogram. Circulation. 1969;39:531–539.
View at Publisher | View at Google Scholar - Das MK, Khan B, Jacob S, et al. (2006). Significance of a fragmented QRS complex versus a Q wave in patients with coronary artery disease. Circulation. 2006;113:2495–2501.
View at Publisher | View at Google Scholar - Elsayed YMH. (2020). Electrocardiographic Passing Phenomenon (Flying Phenomenon or Yasser’s Phenomenon) Conveys the Traditional Cardiovascular Management; Interpretations and Reassurance; Retrospective Observational Study. Anaest & Sur Open Access J. 1(3): 2020. ASOAJ.MS.ID.000515.
View at Publisher | View at Google Scholar
Dear Grace Pierce, Editorial Coordinator of Journal of Clinical Research and Reports, Thank you for the speedy and efficient peer review process. I appreciate the fact that your peer reviewers do not take months to respond like with some other journals. I would also like to thank the editorial office for responding quickly to my questions. It is an excellent journal. I plan to submit more manuscripts in the future. Best wishes from, Robert W. McGee

Robert W McGee
Dear Grace Pierce, Editorial Coordinator of Journal of Clinical Research and Reports, Working with you and your team on our recent publication in JCRR has been a truly wonderful and enjoyable experience. The responses were prompt, and the reviewers were patient, constructive, and highly professional. One reviewer in particular gave me the feeling that a professor was carefully reading and commenting on my coursework, which was deeply touching. The entire process was straightforward and hassle‑free, with no tedious online forms to complete. I highly recommend this journal. Best wishes from, DR Aibing Rao, Head of R&D

Aibing Rao
I Appreciate the Opportunity to Share my Experience with the Journal of Clinical Research and Reports. The peer review process was timely and constructive, and the feedback provided helped improve the quality of our manuscript. The editorial office was professional, responsive, and supportive throughout the process, ensuring smooth communication and efficient handling of the submission. Overall, it was a positive experience collaborating with your team.

Kashani Mehdi
Dear Mercy Grace, Editorial Coordinator of Obstetrics Gynecology and Reproductive Sciences, We would like to express our gratitude for your help at all stages of publishing and editing the article. The editors of the magazine answer all the necessary questions and help at every stage. We will definitely continue to cooperate and publish other works in the Obstetrics Gynecology and Reproductive Sciences! Best wishes from, Alla Konstantinovna Politova,

Alla Konstantinovna Politova
Dear Maria Emerson, Editorial Coordinator of International Journal of Clinical Case Reports and Reviews, What distinguishes International Journal of Clinical Case Report and Review is not only the scientific rigor of its publications, but the intellectual climate in which research is evaluated. The submission process is refreshingly free of unnecessary formal barriers and bureaucratic rituals that often complicate academic publishing without adding real value. The peer-review system is demanding yet constructive, guided by genuine scientific dialogue rather than hierarchical or authoritarian attitudes. Reviewers act as collaborators in improving the manuscript, not as gatekeepers imposing arbitrary standards. This journal offers a rare balance: high methodological standards combined with a respectful, transparent, and supportive editorial approach. In an era where publishing can feel more burdensome than research itself, this platform restores the original purpose of peer review — to refine ideas, not to obstruct them Prof. Perlat Kapisyzi, FCCP PULMONOLOGIST AND THORACIC IMAGING.
Perlat Kapisyzi
Dear Reader: We have published several articles in the Auctores Publishing, LLC, journal, Clinical Medical Reviews and Reports in recent years (CMRR). This is an ‘open access’ journal and the following are our observations. From the initial invitation to submit an article, to the final edits of galley proofs, we have found CMRR personnel to be professional, responsive, rapid and thorough. This entire process begins with Catherine Mitchell, Editorial Coordinator. She is simply outstanding, and, I believe, unparalleled in her capacity. I cannot imagine a more responsive and dedicated Editorial Coordinator. As I read the dates and timing of her correspondence with us, it seems that she never sleeps. I hope Auctores Publishing, LLC, appreciates her efforts as much as these authors do. Thank you to Auctores Publishing, LLC, to the Editorial Staff/Board, and to Catherine Mitchell from a grateful author(s).