AUCTORES
Globalize your Research
Research | DOI: https://doi.org/10.31579/2690-8794/254
Anthony Kodzo-Grey Venyo, Recently retired UK Clinician, P.O. Box LG 213, Legon, University of Ghana. Legon, Accra, Ghana.
*Corresponding Author: Anthony Kodzo-Grey Venyo, Recently retired UK Clinician, P.O. Box LG 213, Legon, University of Ghana. Legon, Accra, Ghana.
Citation: Grey Venyo AK, (2025), Endometriosis of the Kidney and the Urinary Tract Organs an Update, Clinical Medical Reviews and Reports, 7(2); DOI:10.31579/2690-8794/254
Copyright: © 2025, Anthony Kodzo-Grey Venyo. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 20 February 2025 | Accepted: 27 February 2025 | Published: 07 March 2025
Keywords: endometriosis; kidney; renal pelvis; ureter; urinary bladder; urethra; biopsy; histopathology; radiology image; ultrasound scan; nephrostomy; excision; minimal invasive procedure; laparoscopy
Endometriosis of urogenital tract organs includes the presence of endometrial glands and stroma within or encompassing the urethra, the urinary bladder, the ureters, the renal pelvis or the kidney. Traditionally, endometriosis of the urinary tract had been iterated to be a rare clinical entity with an incidence of 1% to 5.5% in patients with endometriosis. Nevertheless, some authors had indicated that endometriosis of the urinary tract afflicts the kidney and urinary tract organs more frequently than had been previously presumed, particularly in the scenario of patients who have been afflicted by deep infiltrating endometriosis. It had been iterated in a publication previously that ureteric involvement in of endometriosis had been observed in 14.2% of 315 patients with endometriosis. Other authors in the past had documented a prevalence of urinary tract endometriosis of 19.5% in 221 patients with deep infiltrating endometriosis. These previous documentations may indicate that that the prevalence of urinary tract endometriosis had often been underestimated. In view of the fact that endometriosis of the urethra, urinary bladder, ureter, and the kidney manifests with non-specific symptoms and signs, the diagnosis and management of urinary tract endometriosis had remained a challenge. Early diagnosis of endometriosis afflicting the kidney and urinary tract organs is crucial for the prognosis. When the diagnosis is delayed, endometriosis of the ureter could emanate in the development of serious complications such as stenosis of the ureter, with hydroureter and hydronephrosis and finally loss of kidney function. Some cases of endometriosis had tended to be treated with medicaments; nevertheless, surgery has been regarded as the gold standard in the treatment of patients who had been afflicted by deep infiltrating endometriosis. Many publications had demonstrated the feasibility, effectiveness, as well as safety of the laparoscopic approach. In the case of endometriosis of the ureter, the objective of the treatment has tended to be the release of the ureter from all endometriotic tissue to enable normal function and to avoid morbidity. In the scenario of ureteric obstruction by endometriosis, some of the initial management options do include insertion of per-cutaneous nephrostomy or insertion of retrograde ureteric stent to maintain renal function preceding the undertaking of definite treatment procedures. Some cases of endometriosis of the ureter had been managed by ureterolysis; nevertheless, it has remained controversial whether ureterolysis is sufficient or whether more invasive methods such as ureterectomy are necessary to prevent recurrence. Treatment of endometriosis of the urinary has tended to consist of complete surgical excision of the urinary bladder lesion. Some authors had pointed out that partial cystectomy does appear to be superior to the undertaking of trans-urethral resection of the urinary bladder lesion demonstrating lower recurrence rates. With the development of minimal invasive surgical procedures, other options that had recently been undertaken by some authors and could be undertaken in the future by other clinicians to attain effective initial results include: cryotherapy, radiofrequency ablation, irreversible electroporation, thermotherapy, and selective angiography and super-selective embolization of the arterial branch supplying the endometriosis lesion if a pathology examination is obtained from biopsy of the specimen preceding the definitive procedure. The manifesting symptoms of urogenital endometriosis are often non-specific. In view of the possibility of serious complications, clinicians including urologists need to be aware of endometriosis of the kidney and urinary tract organs and its management options. Establishment of pre-operative diagnosis of endometriosis of the kidney and urinary tract organs might help in the planning of intra-operative management of the lesion.
Endometriosis is a terminology that is used for the presence of ectopic endometrial tissue outside the myometrium. [1] Endometriosis is iterated to afflict 10% to 15% of premenopausal women, who are aged usually between 30 years and 35-years. [1] [2] It has been stated that the median age for diagnosis of extragenital lesions is between 35 years and 40 years, which is about 5 years older than that of genital tract lesions. [1] [3] [4] It has been pointed out that extra genital endometriosis may afflict any tissue. [1] It has also been stated that endometriosis afflicting the renal tract is rare and is usually associated with evidence of previous pelvic endometriosis. Endometriosis of the kidney and upper urinary tract is very rare. It had been pointed out that Marshall [5] had described the first case of renal endometriosis. [1] It has furthermore, been iterated that less than 25 cases of renal endometriosis of the kidney had been reported previously in the literature. [1] Endometriosis of the kidney, and upper urinary tract manifests with non-specific symptoms and signs and without a high-index of suspicion, there is a possibility that the diagnosis could be either delayed or the lesion could be misdiagnosed.
Aim
To update the literature of endometriosis of the kidney and upper urinary tract organs.
Methods
Internet databases were searched including: Google; google scholar; yahoo; and PUBMED. The search words that were used included: Endometriosis; Endometriosis of kidney; Renal endometriosis; endometriosis of renal pelvis; endometriosis of ureter; and ureteric endometriosis; endometriosis of bladder; endometriosis of urethra. Seventy-six (76) references were identified which were used to write the article in two parts: (A) Overview, and (B) Miscellaneous narrations and discussions from some case reports, case series, and studies related to endometriosis of the kidney and upper urinary tract organs.
Results
[1] OVERVIEW
Definition / general statement
Essential features
Terminology
It has been iterated that the ensuing terminologies had been used for endometriosis: [6]
Epidemiology
The epidemiology of endometriosis had been summated as follows: [6]
Sites
The sites of the human body that tend to be affected by endometriosis had been summated as follows: [6]
Pathophysiology
The pathophysiology of endometriosis had been summated as follows: [6]
Aetiology
The ensuing iteration had been made regarding the aetiology of endometriosis: [6]
Clinical features
The clinical manifestations of endometriosis had been summated to include the ensuing: [6]
Diagnosis
The diagnosis of endometriosis had been summated as follows: [6]
Radiology description
The radiology-imaging description of endometriosis had been summated as follows: [6]
Prognostic factors
Factors of prognostication associated with endometriosis had been summated as follows: [6]
Treatment
The treatment of endometriosis had been stated to include the ensuing: [6]
Gross description
Macroscopy examination features of endometriosis had been summated as follows: [6]
Frozen section description
Frozen section examination features of specimens containing endometriosis had been summated as follows: [6]
Microscopic (histologic) description
The microscopy pathology examination features of specimens of endometriosis had been summated as follows: [6]
Cytology description
Some of the cytology descriptions of endometriosis that had been reported in various structures had been summated as follows: [6]
Positive stains
It has been stated that immunohistochemistry staining studies of specimens of endometriosis demonstrates positive staining for the ensuing tumour markers: [6]
Molecular / cytogenetics description
Molecular / cytogenetics features of endometriosis had been summated as follows: [6]
Differential diagnoses
Differential diagnoses of endometriosis afflicting some organs had been summated as follows: [6]
[B] Miscellaneous Narrations And Discussions From Some Case Reports, Case Series, And Studies Related To Endometriosis Of The Kidney And Urinary Tract Organs
[1] reported a-38-year-old-woman mother of 2 children, who was diagnosed to have thyrotoxicosis 3 months earlier and who was on carbimazole. She manifested with abdominal pain of 2 months duration and she was found to have left ovarian mass that measured 15 cm x 12 cm x 6 cm in size. Prior to her admission she underwent exploratory laparotomy with bilateral salpingo-oophorectomy and she was referred to the urology team for further management with the surgical specimen. She did not have any menstrual irregularities, dysmenorrhea or urinary symptoms. On examination, she was found to be toxic, sick looking, febrile and she had a pulse rate of 102/min, blood pressure 110/70 mm Hg, and body mass index of 12.4 kg/m2. She had a grade II goitre without any pressure symptoms. Her systemic examination was noted to be unremarkable except for the finding of a lower midline scar over her abdomen, which was infected with an intra-abdominal swelling. The results of her laboratory test examinations demonstrated a hemoglobin of 11 gm/dl, total leukocyte count of 12,000/mm, creatinine 1.33 mg/dl. Her urine routine examination revealed 12-14 pus cells per high power fields and the urine culture grew Escherichia coli. Her T3, T4 and thyrotropin were 2.56 ng/dl [0.6-1.81], 135 ng/dl (45-109), and 0.04 µIU/ml (0.35-5.5). Her thyroid microsomal antibody was positive. A 99mTc-scintigraphy of thyroid and whole-body iodine scan demonstrated diffusely increased uptake of tracer in the thyroid bed. A contrast enhanced CT scan of the abdomen was undertaken to look for intra-abdominal collections which demonstrated an enlarged right kidney with a multiple focal-hypodense lesions of varying sizes (5-10 mm) (see Figure 1), and bilateral inflammatory collections in the adnexal area. The right ureter and pelvis-caliceal system were dilated up to the lower end. The surgical specimen of ovary and fine needle aspiration cytology (FNAC) from hypodense areas of kidney showed evidence of endometriosis (Figure 2). She was administered parenteral antibiotics and she underwent pigtail drainage of intraabdominal collection. Subsequently, she received 5 mci of 131I. During her post-operative 6 weeks follow-up assessment she was found to be euthyroid. An intravenous pyelography was undertaken, and no ureteric obstruction was identified. Danazol of 400gms were orally administered and she was responding very well.
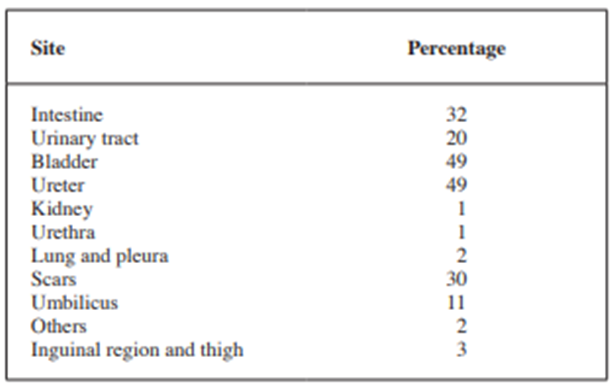
Table 1: Incidence of extra-genital endometriosis at different sites. Reproduced from [1] Under the Creative Commons Attribution License.
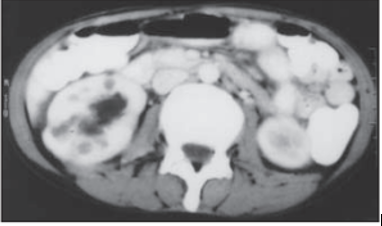
Figure 1: Contrast enhanced Ct scan of the abdomen showing multiple hypodense areas in the right kidney. Reproduced from [1] Under the Creative Commons Attribution License.
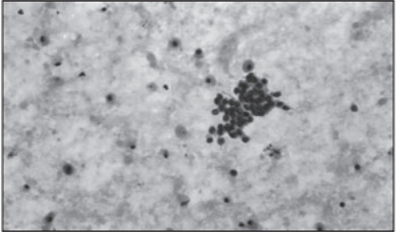
Figure 2: Photomicrograph showing cluster of tubular epithelial cells in a background containing many scattered foamy histiocytes some of which contain hemosiderin. (hematoxylin & eosin x 360). Reproduced from [1] Under the Creative Commons Attribution License.
[1] made the ensuing discussing iterations:
Dutta et al. [1] made the ensuing conclusions:
Ponticelli et al. [38] made the ensuing iterations:
Nezhat et al. [39] made the ensuing iterations:
Nezhat et al. [39] reported 3 cases of endometriosis of the ureter in which there was documentation of renal atrophy and function loss with subsequent workup and surgical intervention. Nezhat et al. [39] stated that the cases had illustrated varying surgical approaches tailored to localization of ureteral endometriosis. All cases were carried out laparoscopically. Nezhat et al. [39] made the ensuing conclusions:
Cheng et al. [40] reported a 53-year-old Chinese premenopausal woman, who had manifested with intermittent right flank pain for many years. She had radiology-imaging studies, which demonstrated a contracted non-functioning right kidney and a perinephric abscess. The contracted kidney was adjudged to have resulted from chronic pyelonephritis. The abscess was drained. The patient subsequently underwent a right nephrectomy. Histopathology examination of the nephrectomy specimen revealed endometriosis of renal parenchyma in addition to xanthogranulomatous pyelonephritis and a perinephric abscess. No evidence of endometriosis was identified within the pelvic site. The patient was symptom-free pursuant to the operation. Cheng et al. [40] made the ensuing conclusions:
Horn et al. [41] stated the following:
Horn et al. [41] reported a 49-year-old woman, who had manifested with a history of abdominal hysterectomy without adnexae because of uterus myomatosus without any signs of endometriosis 6 years earlier. She six years subsequently complained of dysuria and intermittent left loin pain. She had ultrasound scan and retrograde pyelography which demonstrated incomplete ureteric obstruction and her scintigraphy demonstrated a partial loss of kidney function. Intraoperatively frozen section histology examination and final histopathology examination demonstrated a tumorlike intrinsic form of ureteral endometriosis engulfing the left ureter. The patient was treated with uretero-ureterostomy and danazole for preventing recurrence. She was well 28 months post-operatively. Horn et al. [41] made the ensuing conclusion:
Chen et al. [42] stated that endometriosis, mainly occurs in female pelvic organs and that endometriosis in the kidney is extremely rare. Chen et al. [42] reported a case of a 19-year-old girl who had occasional mild abdominal pain that was associated with an ectopic left kidney. She had SPECT-CT scan which showed no abnormal radioactive distribution in the left pelvis, indicating loss of function of the ectopic kidney. Laparoscopic left ectopic kidney resection was subsequently undertaken. Histopathology examination of the excised specimen revealed endometriosis of the ectopic left kidney. Chen et al. [42] concluded that:
Giambelluca et al. [43] made the ensuing iterations:
Giambelluca et al. [43] reported two cases of patients with renal cystic lesions, which were incidentally found by radiology imaging techniques during oncologic follow-up for gastric sarcoma and melanoma, which was initially misinterpreted as complicated haemorrhagic cysts and then histologically characterized as renal localizations of extragenital endometriosis. Giambelluca et al. [43] made the ensuing discussions and conclusions:
Katsikasos et al. [44] stated that renal endometriosis is an uncommon disorder of cases of urinary tract endometriosis. Katsikatsos et al. [44] reported a-42-year-old woman, who presented at their outpatient department with an incidental painless mass upon her left hypoplastic kidney which was demonstrated on an abdominal ultrasound scan. She had abdominal and pelvic examinations which revealed no abnormal findings. She had a computed tomography (CT) scan which showed an anterolateral slightly enhanced left renal mass which measured 1.2 cm in diameter. In addition, the CT scan did not reveal any evidence of abdominal or thoracic metastasis. Katsikatsos et al. [44] stated also that there were a few case reports in the literature of tumours in specimens from patients who had undergone nephrectomy for hypoplastic kidneys, but discriminating between benign and malignant masses is difficult unless a nephrectomy is undertaken. Given the radiological findings and the impaired function of the hypoplastic kidney, laparoscopic radical nephrectomy was recommended. The procedure was undertaken under general anaesthesia without intraoperative or postoperative complications. Microscopy examination of the excised specimen revealed many findings that were consistent with a diagnosis of renal endometriosis. The patient had no symptoms during her last follow-up visit. Katsikatsos et al. [44] concluded that:
Huang et al. [45] undertook a study to determine the risk of chronic kidney disease (CKD) among women with endometriosis in Taiwan. Huang et al. [45] undertook a retrospective cohort study using the National Health Insurance Research Database of Taiwan. Huang et al. [45] selected a total of 27,973 women with a diagnosis of endometriosis and 27,973 multivariable-matched controls (1:1) from 2000 to 2010. Huang et al. [45] reported that Cox regression and computed hazard ratios (HR) with 95% confidence intervals (95% CI) were utilised to determine the risk of CKD among women with endometriosis. Huang et al. [45] summated the results as follows:
Huang et al. [45] made the ensuing conclusions:
Gagnon et al. [46] reported a 27‐year‐old woman, who was known to have a solitary left kidney since the age of 17 years. In her early 20s she was investigated for recurrent lower abdominal pain that was related to her menstrual periods. At the age of 25 years (in 1997), her pain within the right inguinal area was explored surgically, and endometriosis within the proximity of the round ligament was found and excised. Her cyclic pelvic pain was investigated further and a laparoscopy demonstrated endometriosis within the Douglas pouch. The patient was also known to have a bicornuate uterus, which was considered to be a risk factor for endometriosis. While waiting for definitive surgery of pelvic endometriosis (in December 1997), she manifested with recurrent episodes of fever, anorexia, nausea and fatigue accompanied by pelvic pain beginning in the middle of her menstrual periods and lasting for a few days afterwards. She had noted progressive polyuria and nocturia. She came to medical attention in April 1998, during a more severe cyclic episode in which she manifested with vomiting and headache. She was found to be severely hypertensive (blood pressure 200/120) with an elevated serum creatinine at 201 μmol/l (baseline value of 89 μmol/l in 1989). An ultrasound was undertaken which showed hydronephrosis of the solitary left kidney with hydroureter. A retrograde pyelogram was undertaken which demonstrated severe obstruction of the distal ureter of the solitary kidney. A double J catheter was advanced with difficulty into the left ureter through the tight distal stenosis. Her clinical symptoms corrected readily together with improvement in her serum creatinine level.
Alhindawi et al. [47] made the ensuing iterations:
Alhindawi et al. [47] reported a 29-year-old woman, who presented with severe deep infiltrating endometriosis resulting in bilateral hydronephrosis and loss of left kidney function. She underwent laparoscopic excision of deep infiltrating endometriosis, ureterolysis, bowel resection and colostomy formation. Eventually the left non-functional kidney required nephrectomy. Alhindawi et al. [47] made the ensuing conclusions:
Carmignani et al. [48] assessed whether routine renal ultrasound scan may be recommended in all patients with pelvic endometriosis, in order to avoid silent ureteral involvement of the disease. Carmignani et al. [48] undertook a retrospective descriptive study on seven hundred and fifty patients with a primary diagnosis of endometriosis, between January 2005 and July 2007. Routine urinary ultrasound; recording of patient history, signs, and symptoms; gynecologic examination; blood and urinary analyses; magnetic resonance imaging; spiral multi-slice computerized tomography, were undertaken. Carmignani et al. [48] summated the results as follows:
Carmignani et al. [48] made the ensuing conclusion(s):
Arrieta Bretón et al. [49] reported on the impact that urinary tract endometriosis may have on renal function. They stated that ureteral endometriosis is an uncommon and a silent cause of renal injury as well as that it is therefore very important to be highly suspicious in order to be able to make an early diagnosis and thus prevent renal failure. Arrieta Bretón et al. [49] reported on cases documenting on the management and outcome of three cases of premenopausal women with deep endometriosis affecting the ureter, associated with secondary unilateral complete loss of renal function. Arrieta Bretón et al. [49] summated the results with conclusions as follows:
Langebrekke and Qvigstad [50] made the ensuing iterations:
Langebrekke and Qvigstad [50] reported on three patients with loss of renal function, in whom different pathogenic mechanisms probably were the decisive cause. Langebrekke and Qvigstad [50] stated the following:
Yohannes [51] undertook a comprehensive literature review of reports on the diagnosis and management of ureteral endometriosis was performed using MEDLINE. Yohannes [51] summated the results as follows:
Yohannes [51] made the ensuing conclusions:
Pérez et al. [52] undertook a retrospective analysis of 12 cases of urinary tract endometriosis diagnosed from 1993 to 2008. Pérez et al. [52] summated the results as follows:
Pérez et al. [52] made the ensuing conclusions:
Knabben et al. [53] analysed the prevalence of urinary tract endometriosis (UTE) in patients with deep infiltrating endometriosis (DIE) in order to define potential criteria for preoperative workup. Knabben et al. [53] undertook a retrospective study of six hundred and ninety-seven patients with endometriosis who underwent excision of all endometriotic lesions. Knabben et al. [53] undertook a correlation of preoperative features and intraoperative findings in patients who had UTE. Knabben et al. [53] summated the result(s) as follows:
Knabben et al. [53] made the ensuing conclusion:
Badri et al. [54] made the ensuing iterations:
Badri et al. [54] reported the case of a 45-year-old woman with flank pain and haematuria, who was found to have a left kidney mass on cross-sectional imaging. After robotic partial nephrectomy was undertaken, pathology analysis of the specimen revealed an endometrial implant within the renal parenchyma. Badri et al. [54] concluded that:
Gabriel et al. [55] reported on the prevalence, surgical management, and outcome of urinary tract endometriosis (UTE) in a cohort of 221 patients who had undergone laparoscopic surgery for severe endometriosis. They stated that UTE can cause significant morbidity, such as silent kidney or progressive renal function loss and that its frequency is underestimated and data on laparoscopic management are scarce. Gabriel et al. [55] undertook a retrospective study between 2007 and 2010, of 43 patients who were eligible for their single-centre study. The inclusion criterion was the presence of UTE (for example urinary bladder and/or ureteric endometriosis). All patients were operated laparoscopically. Gabriel et al. [55] summated the results as follows:
Gabriel et al. [55] made the ensuing conclusions:
Muthuppalaniappan et al. [56] reported a case of a 30-year-old female, who had a background history of SLE with a silent progressive kidney injury due to an obstructive uropathy secondary to bilateral intrinsic UE and severe loss of her left kidney function that was treated with ureteric stenting. She subsequently underwent bilateral re-implantation of her ureters as a definitive treatment plan as she had expressed a desire to conceive.
Muthuppalaniappan et al. [56] made the ensuing discussing iterations:
Muthuppalaniappan et al. [56] made the ensuing conclusions:
Vrettos et al. [57] made the ensuing iterations:
[57] reported a case of a 43-year-old lady who manifested with recurrent episodes of right-sided colicky abdominal pain. She manifested with severe, right-sided colicky abdominal and right loin pain which radiated to the right groin. She reported similar episodes of pain previously, but no clear diagnosis had been established. Her primary care physician had treated her conservatively for possible kidney stones, even though there was no radiology-image evidence to support that. Upon examination, she was found to be afebrile and her vital signs were stable. Her blood results demonstrated a mild elevation in her urea and creatinine levels. She had a computed tomography scan of the kidneys-ureter-bladder (CT KUB), which showed a moderate degree of right sided hydronephrosis but no stone was identified (see figure 3). An intravenous urogram (IVU) was undertaken which demonstrated marked distension of the right pelvic calyceal system and narrowing of the right distal ureter (see figure 3). The patient then subsequently had a magnetic resonance imaging (MRI) scan which demonstrated abnormal soft tissue thickening within the right adnexal region, but no clear cause of the ureteric obstruction was demonstrated (see figure 4). She then underwent laparoscopy to ascertain the nature of the pathology and to provide tissue diagnosis. The pathology findings demonstrated elements of endometrial tissue which had encased the distal ureter. In view of the proximity of the ureteric stenosis to the ureterovesical junction, the patient was treated by means of an open ureterocystoneostomy. She had an uncomplicated course and her pain resolved after the operation. She did not experience any further episodes of pain. She had been followed up as an outpatient regularly with monitoring of her renal function, which had remained normal and stable.
Figure 3: Computed tomography scan of the kidneys-ureter-bladder (CT KUB) demonstrating right sided hydronephrosis (arrow). Intravenous urogram (IVU) showing narrowing of the right distal ureter (arrowhead). Reproduced from [57] Under the Creative Commons Attribution License.
Figure 4: Magnetic resonance imaging (MRI) scan of the pelvis showing abnormal tissue (arrowhead) which encases the right distal ureter (arrow). Reproduced from: [57] Under the Creative Commons Attribution License.
[57] made the ensuing discussions and conclusions:
[67] made the ensuing iterations:
[68] made the ensuing iterations:
Nagar et al. [68] reported a 30 years old healthy woman, who was admitted due to abdominal pain lasting for 5 days without fever. She complained of dysmenorrhea but no other gynaecological, urinary or digestive symptoms. She had trans vaginal + abdominal ultrasound (US) of a left ovarian unilocular cyst that measured 85*83*123mm with “ground glass” content, which was suspected for endometrioma. Severe hydronephrosis of left kidney with dilated calyx and cortical thinning, pelvic tubular structure 30*18 with clear fluid was suspected for dilated left hydroureter. Under radiology-imaging limitations there were no signs of DIE CT UROGRAPHY was undertaken which confirmed the urinary system findings. Her laboratory test serum creatinine was 0.79, the results of her electrolytes were normal. Surgery (laparoscopy) drainage of 10cm left endometrioma, left salpingectomy due to LT hydrosalpinx, removal of 4cm deep infiltrating endometriotic nodule that involved the left ureter, left uterine artery and left infundibulo-pelvic ligament was and left were nephroureterectomy undertaken.
[68] made the ensuing conclusions:
[69] presented data from 18 cases of ureteral endometriosis. They undertook Prospective clinical study of four hundred and five patients with severe dysmenorrhea or deep dyspareunia due to a rectovaginal endometriotic (adenomyotic) nodule. The patients were prospectively evaluated using intravenous pyelography. All of the patients underwent laparoscopic surgery to remove rectovaginal adenomyosis and ureterolysis. The main outcome measure included presurgical and postsurgical evaluation and histological analysis.[69] summated the result(s) as follows:
They made the ensuing conclusion(s):
[70] reported a-29-year-old woman, who manifested with unilateral loin pain because of severely hydro-nephrotic kidney due to deposits of pelvic endometriosis. Double J-stent was inserted beyond the obstruction and she was commenced on hormone therapy. The stent was removed after three months when her back pressure changes had resolved. Gupta et al. [70] concluded that the case was presented along with a short relevant discussion, due to rarity of ureteral involvement by endometriosis.
[71] reported a 42-year-old woman, who was referred to their hospital because of abdominal fullness and a large abdominal mass and other symptoms. She had computed tomography (CT) scan and retrograde pyelography (RP) which revealed left hydronephrosis and a filling defect in the left lower ureter. Based on the diagnoses of endometriosis of bilateral ovaries, uterine myoma and a left ureteral tumour, abdominal total hysterectomy, right salpingo-oophorectomy and partial ureterectomy were undertaken. Pathologically, within the uterus, both leiomyoma and adenomyosis, and endometriosis of the right ovary and ureter were diagnosed. Medication with buserelin acetate was commenced.
[72] stated that deep endometriosis (DE) could be more aggressive than other-types of endometrioses, and might even lead to irreversible severe complications such as complete unilateral loss of kidney function. Martinez-Zamora et al. [72] described the clinical and radiology-image characteristics of DE patients who were diagnosed with irreversible unilateral loss of renal function due to unilateral ureteral stenosis and they evaluated risk factors for developing this loss. The study of Martinez-Zamora et al. [72] was a retrospective cohort study, which included 436 patients who underwent laparoscopic DE surgery. Martinez-Zamora et al. [72] evaluated two groups of patients according to preserved (Non-Renal Loss Group; n = 421) or irreversible unilateral damaged renal function (Renal Loss Group; n = 15). They collected pre-operative epidemiologic variables, clinical characteristics, radiologic findings and surgical treatments of all the patients. They found that the Renal Loss Group had a higher infertility rate and a higher proportion of asymptomatic patients. The following radiology image variables showed statistically significant differences between the two groups: mean endometrioma diameter, the presence of intestinal DE and negative sliding sign. Multivariate analysis showed that infertility, being asymptomatic, having intestinal DE or torus uterinus/uterosacral ligament DE and a negative sliding sign significantly increased the risk of loss of renal function. Martinez-Zamora et al. [72] concluded that:
[73] reported a patient who underwent laparoscopic endometriosis resection with right ureterolysis, left nephrectomy, left salpingo-oophorectomy, lysis of adhesions. Nephrectomy and contralateral ureterolysis and dissection of pelvic spaces for successful resection of endometriosis and maintenance of solitary ureter patency was undertaken in order to preserve remaining kidney function. Colussi et al. [73] made the ensuing conclusions:
[74] made the ensuing iterations:
[74] undertook a retrospective study. The study analysed surgical reports of 11,714 patients who underwent endometriosis laparoscopy, and included only 42 patients with urinary bladder endometriosis. Piriyev et al. [74] summated the results as follows:
[74] made the ensuing conclusions:
[75] made the ensuing iterations:
[75] systematically searched MEDLINE, EMBASE, and Cochrane’s databases for studies that employed percutaneous cryoablation therapy for AWE and reported any of the outcomes of interest. The primary outcome was the reduction in the visual analogue scale (VAS) score after treatment. R Software was used for the statistical analysis. Heterogeneity was assessed using I statistics. They assessed the risk of bias in non-randomized studies of interventions framework for potential bias in each selected study. Kaça do Carmo et al. [75] summated the results as follows:
[75] made the ensuing conclusions and declaration of advances in knowledge:
[76] undertook a study to evaluate the efficacy of percutaneous cryoablation in the treatment of abdominal wall endometriosis (AWE) nodules. Bachour et al. [76] retrospectively included thirty-eight women, who were treated for symptomatic AWE nodules with percutaneous cryoablation under ultrasound and computed tomography (CT) guidance between May 2020 and July 2023. Pain was estimated using visual analog scale (VAS) and assessed at baseline, three months, six months, and 12 months after percutaneous cryoablation. Baseline VAS score, volume of AWE nodule and magnetic resonance imaging (MRI) features of AWE nodules were compared to those obtained after percutaneous cryoablation. Major complications, if any, were noted. Bachour et al. [76] summated the results as follows:
Bachour et al. [76] concluded that:
Conflict Of Interest – Nil
Acknowledgements
Acknowledgements to:
Clearly Auctoresonline and particularly Psychology and Mental Health Care Journal is dedicated to improving health care services for individuals and populations. The editorial boards' ability to efficiently recognize and share the global importance of health literacy with a variety of stakeholders. Auctoresonline publishing platform can be used to facilitate of optimal client-based services and should be added to health care professionals' repertoire of evidence-based health care resources.

Journal of Clinical Cardiology and Cardiovascular Intervention The submission and review process was adequate. However I think that the publication total value should have been enlightened in early fases. Thank you for all.

Journal of Women Health Care and Issues By the present mail, I want to say thank to you and tour colleagues for facilitating my published article. Specially thank you for the peer review process, support from the editorial office. I appreciate positively the quality of your journal.
Journal of Clinical Research and Reports I would be very delighted to submit my testimonial regarding the reviewer board and the editorial office. The reviewer board were accurate and helpful regarding any modifications for my manuscript. And the editorial office were very helpful and supportive in contacting and monitoring with any update and offering help. It was my pleasure to contribute with your promising Journal and I am looking forward for more collaboration.

We would like to thank the Journal of Thoracic Disease and Cardiothoracic Surgery because of the services they provided us for our articles. The peer-review process was done in a very excellent time manner, and the opinions of the reviewers helped us to improve our manuscript further. The editorial office had an outstanding correspondence with us and guided us in many ways. During a hard time of the pandemic that is affecting every one of us tremendously, the editorial office helped us make everything easier for publishing scientific work. Hope for a more scientific relationship with your Journal.

The peer-review process which consisted high quality queries on the paper. I did answer six reviewers’ questions and comments before the paper was accepted. The support from the editorial office is excellent.

Journal of Neuroscience and Neurological Surgery. I had the experience of publishing a research article recently. The whole process was simple from submission to publication. The reviewers made specific and valuable recommendations and corrections that improved the quality of my publication. I strongly recommend this Journal.

Dr. Katarzyna Byczkowska My testimonial covering: "The peer review process is quick and effective. The support from the editorial office is very professional and friendly. Quality of the Clinical Cardiology and Cardiovascular Interventions is scientific and publishes ground-breaking research on cardiology that is useful for other professionals in the field.

Thank you most sincerely, with regard to the support you have given in relation to the reviewing process and the processing of my article entitled "Large Cell Neuroendocrine Carcinoma of The Prostate Gland: A Review and Update" for publication in your esteemed Journal, Journal of Cancer Research and Cellular Therapeutics". The editorial team has been very supportive.

Testimony of Journal of Clinical Otorhinolaryngology: work with your Reviews has been a educational and constructive experience. The editorial office were very helpful and supportive. It was a pleasure to contribute to your Journal.

Dr. Bernard Terkimbi Utoo, I am happy to publish my scientific work in Journal of Women Health Care and Issues (JWHCI). The manuscript submission was seamless and peer review process was top notch. I was amazed that 4 reviewers worked on the manuscript which made it a highly technical, standard and excellent quality paper. I appreciate the format and consideration for the APC as well as the speed of publication. It is my pleasure to continue with this scientific relationship with the esteem JWHCI.

This is an acknowledgment for peer reviewers, editorial board of Journal of Clinical Research and Reports. They show a lot of consideration for us as publishers for our research article “Evaluation of the different factors associated with side effects of COVID-19 vaccination on medical students, Mutah university, Al-Karak, Jordan”, in a very professional and easy way. This journal is one of outstanding medical journal.
Dear Hao Jiang, to Journal of Nutrition and Food Processing We greatly appreciate the efficient, professional and rapid processing of our paper by your team. If there is anything else we should do, please do not hesitate to let us know. On behalf of my co-authors, we would like to express our great appreciation to editor and reviewers.

As an author who has recently published in the journal "Brain and Neurological Disorders". I am delighted to provide a testimonial on the peer review process, editorial office support, and the overall quality of the journal. The peer review process at Brain and Neurological Disorders is rigorous and meticulous, ensuring that only high-quality, evidence-based research is published. The reviewers are experts in their fields, and their comments and suggestions were constructive and helped improve the quality of my manuscript. The review process was timely and efficient, with clear communication from the editorial office at each stage. The support from the editorial office was exceptional throughout the entire process. The editorial staff was responsive, professional, and always willing to help. They provided valuable guidance on formatting, structure, and ethical considerations, making the submission process seamless. Moreover, they kept me informed about the status of my manuscript and provided timely updates, which made the process less stressful. The journal Brain and Neurological Disorders is of the highest quality, with a strong focus on publishing cutting-edge research in the field of neurology. The articles published in this journal are well-researched, rigorously peer-reviewed, and written by experts in the field. The journal maintains high standards, ensuring that readers are provided with the most up-to-date and reliable information on brain and neurological disorders. In conclusion, I had a wonderful experience publishing in Brain and Neurological Disorders. The peer review process was thorough, the editorial office provided exceptional support, and the journal's quality is second to none. I would highly recommend this journal to any researcher working in the field of neurology and brain disorders.

Dear Agrippa Hilda, Journal of Neuroscience and Neurological Surgery, Editorial Coordinator, I trust this message finds you well. I want to extend my appreciation for considering my article for publication in your esteemed journal. I am pleased to provide a testimonial regarding the peer review process and the support received from your editorial office. The peer review process for my paper was carried out in a highly professional and thorough manner. The feedback and comments provided by the authors were constructive and very useful in improving the quality of the manuscript. This rigorous assessment process undoubtedly contributes to the high standards maintained by your journal.

International Journal of Clinical Case Reports and Reviews. I strongly recommend to consider submitting your work to this high-quality journal. The support and availability of the Editorial staff is outstanding and the review process was both efficient and rigorous.

Thank you very much for publishing my Research Article titled “Comparing Treatment Outcome Of Allergic Rhinitis Patients After Using Fluticasone Nasal Spray And Nasal Douching" in the Journal of Clinical Otorhinolaryngology. As Medical Professionals we are immensely benefited from study of various informative Articles and Papers published in this high quality Journal. I look forward to enriching my knowledge by regular study of the Journal and contribute my future work in the field of ENT through the Journal for use by the medical fraternity. The support from the Editorial office was excellent and very prompt. I also welcome the comments received from the readers of my Research Article.

Dear Erica Kelsey, Editorial Coordinator of Cancer Research and Cellular Therapeutics Our team is very satisfied with the processing of our paper by your journal. That was fast, efficient, rigorous, but without unnecessary complications. We appreciated the very short time between the submission of the paper and its publication on line on your site.

I am very glad to say that the peer review process is very successful and fast and support from the Editorial Office. Therefore, I would like to continue our scientific relationship for a long time. And I especially thank you for your kindly attention towards my article. Have a good day!

"We recently published an article entitled “Influence of beta-Cyclodextrins upon the Degradation of Carbofuran Derivatives under Alkaline Conditions" in the Journal of “Pesticides and Biofertilizers” to show that the cyclodextrins protect the carbamates increasing their half-life time in the presence of basic conditions This will be very helpful to understand carbofuran behaviour in the analytical, agro-environmental and food areas. We greatly appreciated the interaction with the editor and the editorial team; we were particularly well accompanied during the course of the revision process, since all various steps towards publication were short and without delay".

I would like to express my gratitude towards you process of article review and submission. I found this to be very fair and expedient. Your follow up has been excellent. I have many publications in national and international journal and your process has been one of the best so far. Keep up the great work.

We are grateful for this opportunity to provide a glowing recommendation to the Journal of Psychiatry and Psychotherapy. We found that the editorial team were very supportive, helpful, kept us abreast of timelines and over all very professional in nature. The peer review process was rigorous, efficient and constructive that really enhanced our article submission. The experience with this journal remains one of our best ever and we look forward to providing future submissions in the near future.

I am very pleased to serve as EBM of the journal, I hope many years of my experience in stem cells can help the journal from one way or another. As we know, stem cells hold great potential for regenerative medicine, which are mostly used to promote the repair response of diseased, dysfunctional or injured tissue using stem cells or their derivatives. I think Stem Cell Research and Therapeutics International is a great platform to publish and share the understanding towards the biology and translational or clinical application of stem cells.

I would like to give my testimony in the support I have got by the peer review process and to support the editorial office where they were of asset to support young author like me to be encouraged to publish their work in your respected journal and globalize and share knowledge across the globe. I really give my great gratitude to your journal and the peer review including the editorial office.

I am delighted to publish our manuscript entitled "A Perspective on Cocaine Induced Stroke - Its Mechanisms and Management" in the Journal of Neuroscience and Neurological Surgery. The peer review process, support from the editorial office, and quality of the journal are excellent. The manuscripts published are of high quality and of excellent scientific value. I recommend this journal very much to colleagues.

Dr.Tania Muñoz, My experience as researcher and author of a review article in The Journal Clinical Cardiology and Interventions has been very enriching and stimulating. The editorial team is excellent, performs its work with absolute responsibility and delivery. They are proactive, dynamic and receptive to all proposals. Supporting at all times the vast universe of authors who choose them as an option for publication. The team of review specialists, members of the editorial board, are brilliant professionals, with remarkable performance in medical research and scientific methodology. Together they form a frontline team that consolidates the JCCI as a magnificent option for the publication and review of high-level medical articles and broad collective interest. I am honored to be able to share my review article and open to receive all your comments.

“The peer review process of JPMHC is quick and effective. Authors are benefited by good and professional reviewers with huge experience in the field of psychology and mental health. The support from the editorial office is very professional. People to contact to are friendly and happy to help and assist any query authors might have. Quality of the Journal is scientific and publishes ground-breaking research on mental health that is useful for other professionals in the field”.

Dear editorial department: On behalf of our team, I hereby certify the reliability and superiority of the International Journal of Clinical Case Reports and Reviews in the peer review process, editorial support, and journal quality. Firstly, the peer review process of the International Journal of Clinical Case Reports and Reviews is rigorous, fair, transparent, fast, and of high quality. The editorial department invites experts from relevant fields as anonymous reviewers to review all submitted manuscripts. These experts have rich academic backgrounds and experience, and can accurately evaluate the academic quality, originality, and suitability of manuscripts. The editorial department is committed to ensuring the rigor of the peer review process, while also making every effort to ensure a fast review cycle to meet the needs of authors and the academic community. Secondly, the editorial team of the International Journal of Clinical Case Reports and Reviews is composed of a group of senior scholars and professionals with rich experience and professional knowledge in related fields. The editorial department is committed to assisting authors in improving their manuscripts, ensuring their academic accuracy, clarity, and completeness. Editors actively collaborate with authors, providing useful suggestions and feedback to promote the improvement and development of the manuscript. We believe that the support of the editorial department is one of the key factors in ensuring the quality of the journal. Finally, the International Journal of Clinical Case Reports and Reviews is renowned for its high- quality articles and strict academic standards. The editorial department is committed to publishing innovative and academically valuable research results to promote the development and progress of related fields. The International Journal of Clinical Case Reports and Reviews is reasonably priced and ensures excellent service and quality ratio, allowing authors to obtain high-level academic publishing opportunities in an affordable manner. I hereby solemnly declare that the International Journal of Clinical Case Reports and Reviews has a high level of credibility and superiority in terms of peer review process, editorial support, reasonable fees, and journal quality. Sincerely, Rui Tao.

Clinical Cardiology and Cardiovascular Interventions I testity the covering of the peer review process, support from the editorial office, and quality of the journal.

Clinical Cardiology and Cardiovascular Interventions, we deeply appreciate the interest shown in our work and its publication. It has been a true pleasure to collaborate with you. The peer review process, as well as the support provided by the editorial office, have been exceptional, and the quality of the journal is very high, which was a determining factor in our decision to publish with you.
The peer reviewers process is quick and effective, the supports from editorial office is excellent, the quality of journal is high. I would like to collabroate with Internatioanl journal of Clinical Case Reports and Reviews journal clinically in the future time.

Clinical Cardiology and Cardiovascular Interventions, I would like to express my sincerest gratitude for the trust placed in our team for the publication in your journal. It has been a true pleasure to collaborate with you on this project. I am pleased to inform you that both the peer review process and the attention from the editorial coordination have been excellent. Your team has worked with dedication and professionalism to ensure that your publication meets the highest standards of quality. We are confident that this collaboration will result in mutual success, and we are eager to see the fruits of this shared effort.

Dear Dr. Jessica Magne, Editorial Coordinator 0f Clinical Cardiology and Cardiovascular Interventions, I hope this message finds you well. I want to express my utmost gratitude for your excellent work and for the dedication and speed in the publication process of my article titled "Navigating Innovation: Qualitative Insights on Using Technology for Health Education in Acute Coronary Syndrome Patients." I am very satisfied with the peer review process, the support from the editorial office, and the quality of the journal. I hope we can maintain our scientific relationship in the long term.
Dear Monica Gissare, - Editorial Coordinator of Nutrition and Food Processing. ¨My testimony with you is truly professional, with a positive response regarding the follow-up of the article and its review, you took into account my qualities and the importance of the topic¨.

Dear Dr. Jessica Magne, Editorial Coordinator 0f Clinical Cardiology and Cardiovascular Interventions, The review process for the article “The Handling of Anti-aggregants and Anticoagulants in the Oncologic Heart Patient Submitted to Surgery” was extremely rigorous and detailed. From the initial submission to the final acceptance, the editorial team at the “Journal of Clinical Cardiology and Cardiovascular Interventions” demonstrated a high level of professionalism and dedication. The reviewers provided constructive and detailed feedback, which was essential for improving the quality of our work. Communication was always clear and efficient, ensuring that all our questions were promptly addressed. The quality of the “Journal of Clinical Cardiology and Cardiovascular Interventions” is undeniable. It is a peer-reviewed, open-access publication dedicated exclusively to disseminating high-quality research in the field of clinical cardiology and cardiovascular interventions. The journal's impact factor is currently under evaluation, and it is indexed in reputable databases, which further reinforces its credibility and relevance in the scientific field. I highly recommend this journal to researchers looking for a reputable platform to publish their studies.
Dear Editorial Coordinator of the Journal of Nutrition and Food Processing! "I would like to thank the Journal of Nutrition and Food Processing for including and publishing my article. The peer review process was very quick, movement and precise. The Editorial Board has done an extremely conscientious job with much help, valuable comments and advices. I find the journal very valuable from a professional point of view, thank you very much for allowing me to be part of it and I would like to participate in the future!”

Dealing with The Journal of Neurology and Neurological Surgery was very smooth and comprehensive. The office staff took time to address my needs and the response from editors and the office was prompt and fair. I certainly hope to publish with this journal again.Their professionalism is apparent and more than satisfactory. Susan Weiner

My Testimonial Covering as fellowing: Lin-Show Chin. The peer reviewers process is quick and effective, the supports from editorial office is excellent, the quality of journal is high. I would like to collabroate with Internatioanl journal of Clinical Case Reports and Reviews.

My experience publishing in Psychology and Mental Health Care was exceptional. The peer review process was rigorous and constructive, with reviewers providing valuable insights that helped enhance the quality of our work. The editorial team was highly supportive and responsive, making the submission process smooth and efficient. The journal's commitment to high standards and academic rigor makes it a respected platform for quality research. I am grateful for the opportunity to publish in such a reputable journal.
My experience publishing in International Journal of Clinical Case Reports and Reviews was exceptional. I Come forth to Provide a Testimonial Covering the Peer Review Process and the editorial office for the Professional and Impartial Evaluation of the Manuscript.

I would like to offer my testimony in the support. I have received through the peer review process and support the editorial office where they are to support young authors like me, encourage them to publish their work in your esteemed journals, and globalize and share knowledge globally. I really appreciate your journal, peer review, and editorial office.
Dear Agrippa Hilda- Editorial Coordinator of Journal of Neuroscience and Neurological Surgery, "The peer review process was very quick and of high quality, which can also be seen in the articles in the journal. The collaboration with the editorial office was very good."

I would like to express my sincere gratitude for the support and efficiency provided by the editorial office throughout the publication process of my article, “Delayed Vulvar Metastases from Rectal Carcinoma: A Case Report.” I greatly appreciate the assistance and guidance I received from your team, which made the entire process smooth and efficient. The peer review process was thorough and constructive, contributing to the overall quality of the final article. I am very grateful for the high level of professionalism and commitment shown by the editorial staff, and I look forward to maintaining a long-term collaboration with the International Journal of Clinical Case Reports and Reviews.
To Dear Erin Aust, I would like to express my heartfelt appreciation for the opportunity to have my work published in this esteemed journal. The entire publication process was smooth and well-organized, and I am extremely satisfied with the final result. The Editorial Team demonstrated the utmost professionalism, providing prompt and insightful feedback throughout the review process. Their clear communication and constructive suggestions were invaluable in enhancing my manuscript, and their meticulous attention to detail and dedication to quality are truly commendable. Additionally, the support from the Editorial Office was exceptional. From the initial submission to the final publication, I was guided through every step of the process with great care and professionalism. The team's responsiveness and assistance made the entire experience both easy and stress-free. I am also deeply impressed by the quality and reputation of the journal. It is an honor to have my research featured in such a respected publication, and I am confident that it will make a meaningful contribution to the field.

"I am grateful for the opportunity of contributing to [International Journal of Clinical Case Reports and Reviews] and for the rigorous review process that enhances the quality of research published in your esteemed journal. I sincerely appreciate the time and effort of your team who have dedicatedly helped me in improvising changes and modifying my manuscript. The insightful comments and constructive feedback provided have been invaluable in refining and strengthening my work".

I thank the ‘Journal of Clinical Research and Reports’ for accepting this article for publication. This is a rigorously peer reviewed journal which is on all major global scientific data bases. I note the review process was prompt, thorough and professionally critical. It gave us an insight into a number of important scientific/statistical issues. The review prompted us to review the relevant literature again and look at the limitations of the study. The peer reviewers were open, clear in the instructions and the editorial team was very prompt in their communication. This journal certainly publishes quality research articles. I would recommend the journal for any future publications.

Dear Jessica Magne, with gratitude for the joint work. Fast process of receiving and processing the submitted scientific materials in “Clinical Cardiology and Cardiovascular Interventions”. High level of competence of the editors with clear and correct recommendations and ideas for enriching the article.

We found the peer review process quick and positive in its input. The support from the editorial officer has been very agile, always with the intention of improving the article and taking into account our subsequent corrections.

My article, titled 'No Way Out of the Smartphone Epidemic Without Considering the Insights of Brain Research,' has been republished in the International Journal of Clinical Case Reports and Reviews. The review process was seamless and professional, with the editors being both friendly and supportive. I am deeply grateful for their efforts.
To Dear Erin Aust – Editorial Coordinator of Journal of General Medicine and Clinical Practice! I declare that I am absolutely satisfied with your work carried out with great competence in following the manuscript during the various stages from its receipt, during the revision process to the final acceptance for publication. Thank Prof. Elvira Farina

Dear Jessica, and the super professional team of the ‘Clinical Cardiology and Cardiovascular Interventions’ I am sincerely grateful to the coordinated work of the journal team for the no problem with the submission of my manuscript: “Cardiometabolic Disorders in A Pregnant Woman with Severe Preeclampsia on the Background of Morbid Obesity (Case Report).” The review process by 5 experts was fast, and the comments were professional, which made it more specific and academic, and the process of publication and presentation of the article was excellent. I recommend that my colleagues publish articles in this journal, and I am interested in further scientific cooperation. Sincerely and best wishes, Dr. Oleg Golyanovskiy.

Dear Ashley Rosa, Editorial Coordinator of the journal - Psychology and Mental Health Care. " The process of obtaining publication of my article in the Psychology and Mental Health Journal was positive in all areas. The peer review process resulted in a number of valuable comments, the editorial process was collaborative and timely, and the quality of this journal has been quickly noticed, resulting in alternative journals contacting me to publish with them." Warm regards, Susan Anne Smith, PhD. Australian Breastfeeding Association.

Dear Jessica Magne, Editorial Coordinator, Clinical Cardiology and Cardiovascular Interventions, Auctores Publishing LLC. I appreciate the journal (JCCI) editorial office support, the entire team leads were always ready to help, not only on technical front but also on thorough process. Also, I should thank dear reviewers’ attention to detail and creative approach to teach me and bring new insights by their comments. Surely, more discussions and introduction of other hemodynamic devices would provide better prevention and management of shock states. Your efforts and dedication in presenting educational materials in this journal are commendable. Best wishes from, Farahnaz Fallahian.
Dear Maria Emerson, Editorial Coordinator, International Journal of Clinical Case Reports and Reviews, Auctores Publishing LLC. I am delighted to have published our manuscript, "Acute Colonic Pseudo-Obstruction (ACPO): A rare but serious complication following caesarean section." I want to thank the editorial team, especially Maria Emerson, for their prompt review of the manuscript, quick responses to queries, and overall support. Yours sincerely Dr. Victor Olagundoye.

Dear Ashley Rosa, Editorial Coordinator, International Journal of Clinical Case Reports and Reviews. Many thanks for publishing this manuscript after I lost confidence the editors were most helpful, more than other journals Best wishes from, Susan Anne Smith, PhD. Australian Breastfeeding Association.

Dear Agrippa Hilda, Editorial Coordinator, Journal of Neuroscience and Neurological Surgery. The entire process including article submission, review, revision, and publication was extremely easy. The journal editor was prompt and helpful, and the reviewers contributed to the quality of the paper. Thank you so much! Eric Nussbaum, MD